Many will understand the frustrating nature of having to repeat their ‘health story” over and over again to doctors and health providers in different health settings or waiting helplessly while care providers search for information that should be readily available.
Finally, however, it appears that moves are going to be made to potentially decrease these inefficiencies in health settings.
At the MedInfo Congress 2023, held earlier this year in Sydney, Daniel McCabe, Department of Health and Aged Care First Assistant Secretary for Medicare Benefits and Digital Health, announced that in the next 12 months, the Federal Government will introduce legislative changes to mandate the sharing of key health information with consumers by default.

The National Healthcare Interoperability Plan released by the Australian Digital Health Agency is a step towards the interoperability of health data and could have a profound impact on both providers and consumers of health care, including those providing or receiving home or residential aged care.
Mr McCabe said a range of measures will be introduced that will “enable an interconnected healthcare system” and “be supported by consent arrangements to ensure patients choose when and where their information is shared.”
A Council for Connected Care has been established to provide strategic advice to ensure implementation of the plan and garner support for digital health initiatives which he said represents “one of the greatest opportunities we have in Australia to position primary healthcare as a learning and intelligent system that is better at preventing or enabling early interventions to manage health conditions.”
Although there are various degrees of interoperability, secure sharing of health data allows for the efficient exchange of medical records and helps patients receive consistent and coordinated care regardless of where they seek treatment. When data is available live and shared in real-time, individuals can actively participate in their care plans, make informed decisions and monitor their progress more effectively. This not only improves patient satisfaction but also facilitates shared decision-making between patients and healthcare providers.
For those people living or working in home care or residential care settings, health information will be more readily available to caregivers, enabling better decision-making and enhancing overall safety. In home and residential care settings, there may be multiple healthcare providers involved in the patient’s care, such as nurses, doctors, pharmacists, therapists and relatives. Interoperability of health data ensures that all these have access to the same, up-to-date information, improving communication and coordination among the care team.
If a patient needs to transition from one care setting to another, such as from home care to a hospital or vice versa, having their health information readily available ensures a smooth handover and avoids delays in treatment. It also enables healthcare providers to make informed decisions based on the patient’s complete medical history, leading to more personalised and tailored care.
Understanding how their data is collected, stored and shared will empower people to make informed decisions about the level of access they grant to different healthcare providers. With an interoperable health system, individuals can select personal health record (PHR) platforms or apps such as the Touchstone Life Care advance care planning system that allow them to create, store and manage their own health information in a way they choose. These platforms often have features that enable data sharing with authorised healthcare professionals, ensuring that relevant information is readily available when needed. By being proactive in these ways, patients can contribute to the successful implementation of interoperability initiatives and help improve the overall quality of care they receive, whether it be in their home or residential aged care settings.
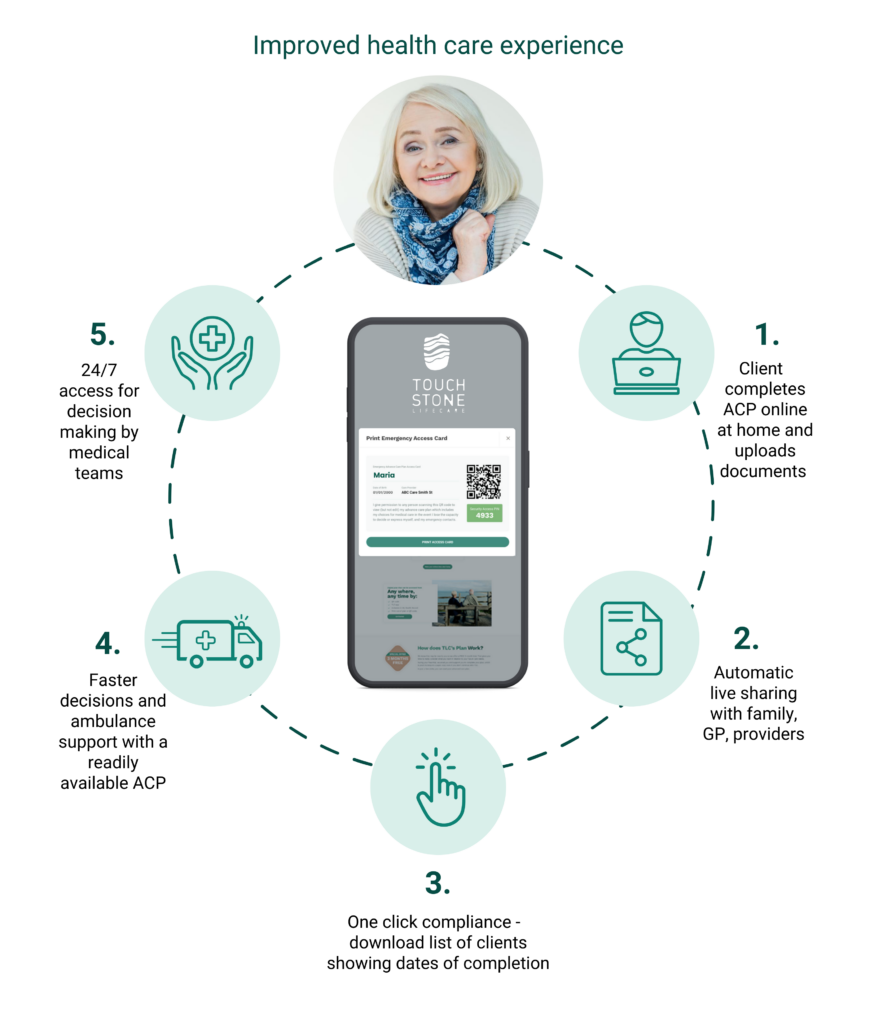
Touchstone Life Care is an example of a company leading this new world of interoperability. The advance care planning platform allows people to create, share and access an interoperable advance care plan. A person can create their plan on a device of their choosing, share it with people they select, and have that plan, or whatever parts of it they choose to share, available to their GP’s desktop, their care facilities’ IT system, on their NDIS provider’s system or as a QR code that paramedics can scan – all as a single source of truth in real-time.
It can connect to smart homes, and wearables, be included in Telehealth consultations, and be uploaded to My Health Record. A person’s wishes and choices about the medical care they want or do not want, are available and accessible 24/7 and instantly, in case they cannot speak for themselves.
Two major tailwinds are driving interoperability throughout the system in general and the aged care system in particular.
1. Care delivered in home and out-of-hospitals driven by:
- An ageing population that is more reluctant to enter residential care.
- A demand for more person-centred care delivered where the person chooses to be.
- The emergence of digitally connected smart homes, wearables, and virtual care.
- The expansion of Commonwealth Home Support and Home Care Packages.
- Consolidation of aged care providers enabling care delivery in retirement villages, with back-to-base alarms and home care available.
2. The need for cost reduction in both health and aged care.
- Governments and health insurers are seeking to reduce the current unsustainable expenditure in health, aged care, and the National Disability Insurance Scheme. Lack of interoperability means time and resources are wasted not only trying to look for data but from the repetition of services that occurs because data is not available.
- Aged care providers are seeking cost reductions to remain financially sustainable. Any tasks that can be completed ahead of admission mean better quality care and coordination after admission.
- The imminent introduction of a user pays aged care model will mean individuals and families will demand more efficient services, care and data management.
Overall, interoperability of health data in home or residential care settings is crucial for ensuring patient safety, improving care coordination, and enabling informed decision-making. Companies such as Touchstone Life Care have been working in this way for several years, and some are yet to come on board. By mandating the sharing of key health information with patients by default, Australia is taking a significant step towards achieving these goals.

Dr Merran Cooper
Dr Merran Cooper MBBS. BSc (Physio), MAICD, M.Admin, PGD Adult Ed is a medical doctor and qualified physiotherapist. In 2018 she responded to the lack of good quality advance care planning in hospitals and the resultant overmedicalisation of dying by founding a technology company, Touchstone Life Care to develop an interoperable, real time advance care planning solution for consumers, providers and health systems.




